The Artemis II mission has captivated me. I find myself checking NASA’s Artemis II Live Mission Coverage on YouTube during in-between moments. So much about this mission astonishes me: The fact that a vehicle is hurtling towards the moon! That there are four people inside! All the math used to plan this trip! That those of us still on Earth get to see and hear the astronauts in almost real-time! (This is the kind of reality TV I can support!) It’s all incredible.
(Let us not forget all the other people who have made this trip possible: The janitors who have kept NASA facilities clean so all staff can think and work in sanitary spaces. The culinary specialists who prepared healthy meals for the astronauts. The accountants who ensured that the mechanics got paid for their work. So many people!)
Within the first day or two, conversations between Houston mission control and the astronauts included the phrase “psychological conferences”. I wondered, “What does this mean?”
When I was in psychiatry residency, a Very Important Person with an Uppity Title at the university hospital was a psychiatrist. When he gave lectures, he routinely shared this perspective:
Psychiatrists have one of the most important jobs in the hospital. Say there are three people in the emergency department. One person is having a heart attack. The second person has a gunshot wound. The third person is trying to grab objects, screaming that they want to kill themselves. Which patient will be the top priority?
(dramatic pause)
The third patient will be the top priority. No one else in the emergency department will be able to receive care safely until that person is de-escalated.
The first time I heard this, I admittedly thought it was self-serving. What a way to puff up psychiatry. However, having witnessed and experienced similar situations, there is truth to what he said.
An emergency department is an enclosed space on Earth with exits to the outdoors. What happens if someone becomes escalated in a capsule in space, thousands of miles from their home planet?
My admiration for NASA has only increased upon finding all the published materials they have about cognition, behaviors, and psychiatric disorders, which are part of their compendium of human system risks. There’s a logic diagram:
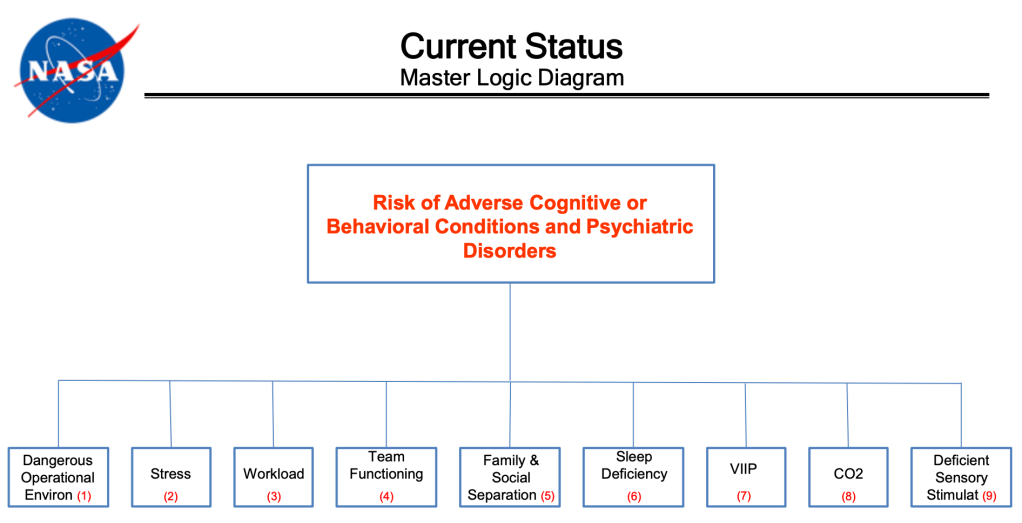
There are likelihood and consequence ratings to measure “Risk of Adverse Cognitive or Behavioral Changes and Psychiatric Disorders Leading to In-mission Health and Performance and Long-term Health Effects“:
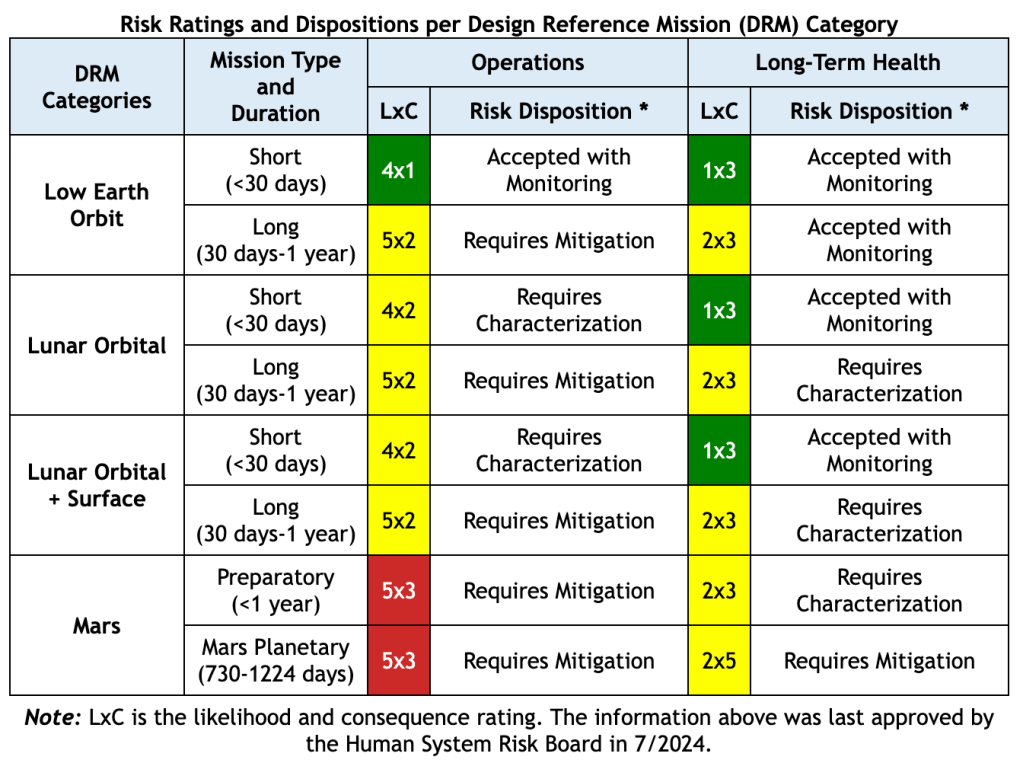
The accompanying 222-page report describes a “behavioral health and performance operational psychology” group that works along the spectrum of prevention, early intervention, and mitigation for astronauts. It looks like flight crews receive robust training in psychological skills (e.g., conflict management, stress management, education about psychology). Further support happens during flight, which we are witnessing now. These include—ah ha!—private psychological conferences, social support from Earth, cognitive monitoring, sleep and circadian rhythm support, team cohesion and care, and looking out the windows. (The authors included the comment, “NASA flight psychiatrists and psychologists have reported that during debriefings astronauts state that they did not realize how important ‘that psych stuff’ was until after they were on the [International Space Station].” This is the story of every psychiatrist and psychologist.)
Furthermore, there are reports about the intersecting psychological risks of “extended duration of isolation and confinement, greater distances from Earth, as well as increased exposures to radiation and altered gravity”. These are well outside the scope of my expertise, but there are lessons from space medicine (!) that NASA has already encouraged all of us on Earth to adopt:

I wish we didn’t have to rely on astronauts to make psychological skills like mindfulness, cognitive restructuring, and maintaining healthy routines sexy, but we’ll take the role models where we can find them!
May the Artemis II voyage be safe and successful. May other people in positions of power and authority learn the patience, cooperation, and discipline from the entire NASA team that made this mission possible.