The ninth, tenth, and eleventh instances of the word “mental” in Project 2025 are on page 875 in the section about the Federal Trade Commission:
Protecting Children Online. The FTC has long protected children in a variety of different contexts. Internet platforms profit from obtaining information from children without parents’ knowledge or consent—and social media’s effect on the well-being of American children is well-documented. Around 2012, American teens experienced a dramatic decline in wellness. Depression, self-harm, suicide attempts, and suicide all increased sharply among U.S. adolescents between 2011 and 2019, with similar trends worldwide. The increase occurred at the same time that social media use moved from rare to ubiquitous among teens, making social media a prime suspect for the sudden rise in mental health issues among teens. In addition, excessive social media use is strongly linked to mental health issues among individuals. Several studies strongly support the notion that social media use is a cause, not just a correlation, of subjective well-being and poor mental health.
This harkens back to the second time the word “mental” appears in the text, where the authors accuse Big Tech of engineering social media for industrial-scale child abuse. The punchline is, yes, the authors of Project 2025 have legitimate and evidence-based concerns about the adverse effects of social media on kids. I appreciate that this section here at least includes people of all ages (i.e., parents) in asserting that “excessive social media use is strongly linked to mental health issues among individuals”.
After this brief foray into children’s mental health, the text veers back towards its point: Trade and contracts.
Targeting children to create potentially harmful contracts or making parents responsible for such contractual relationships is an unfair trade practice.
… leading to this recommendation:
The FTC should examine platforms’ advertising and contract-making with children as a deceptive or unfair trade practice, perhaps requiring written parental consent.
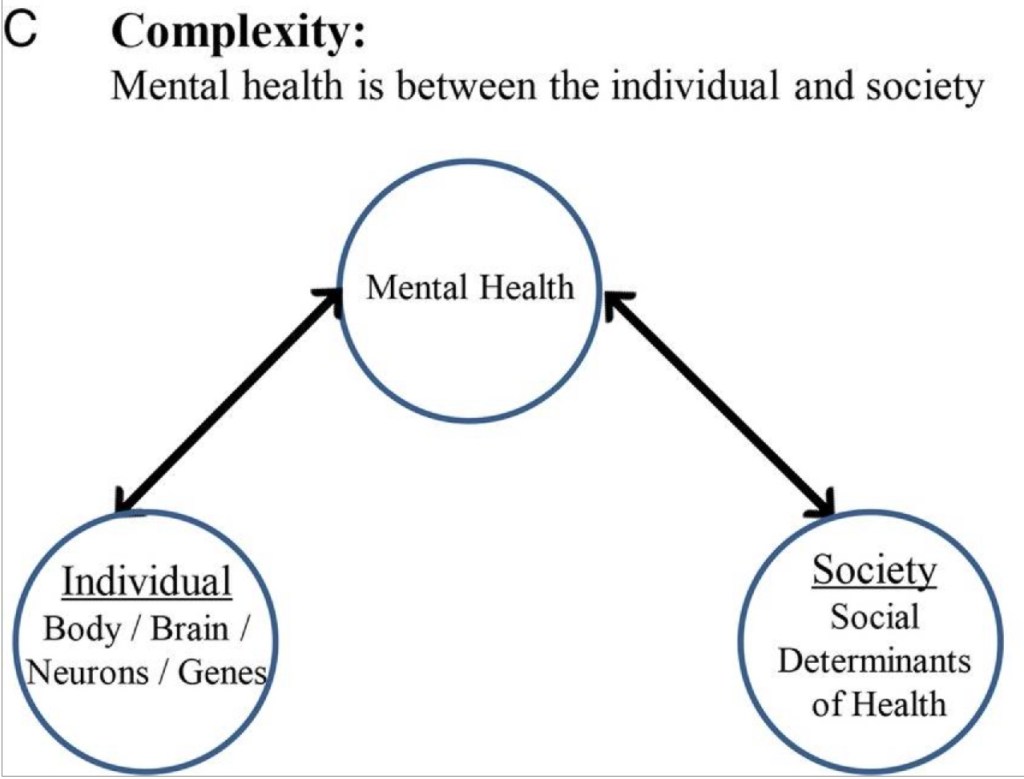
While a perspective of interdependency views everything as being related to everything else, bringing up the mental health of children within the context of the Federal Trade Commission is curious. As we will see in the next instance of the word “mental” in this document (we’re nearing the end — “mental” only shows up 16 times), there’s ambivalence in this chapter about the role of the FTC. Children’s mental health is used chiefly as a potential subject of regulation. Who is better poised to regulate social media and its effects on children? The government? Or parents? Surprisingly, this seems open to debate in this section. (This entire chapter on the FTC uses notably less inflammatory language, too.)
It is clear, just from reviewing the appearance of the word “mental” in this text, that the authors of Project 2025 have opinions about who should have the power and authority to regulate other people. It is apparent who they believe should (cis male, heterosexual fathers) and who should not (women, children, and everyone else). Because Project 2025 makes multiple references to the authority of Judeo-Christian faith, which worships the Father (dude), the Son (dude), and the Holy Ghost (do spirits have genders?), this is presumably why.
Instead of struggling with how to reconcile the agency that all humans can and could have at this current time and place, the authors of Project 2025 have elected an “all or nothing” approach. This is also reflected in the black-or-white, provocative language used in many portions of this enormous document.