The rains have finally returned to Seattle, though the wildfires continue to burn:

That map does not include the entirety of Washington State (there are more fires outside the boundaries of that image), or the fires burning in neighboring Idaho and Oregon.
While we did not experience the blood red skies that San Francisco experienced from the wildfires of the summer of 2020, the air was looked and smelled thick. Each whiff contained fragrant notes of Douglas Fir and perhaps Western Red Cedar, all overwhelmed by charred carbon. Landmarks disappeared into a gritty haze of grey. The evenings featured a crimson sun sinking into ashy layers of peach, pink, and coral.
By October 19th, Seattle had the worst air quality on the planet:
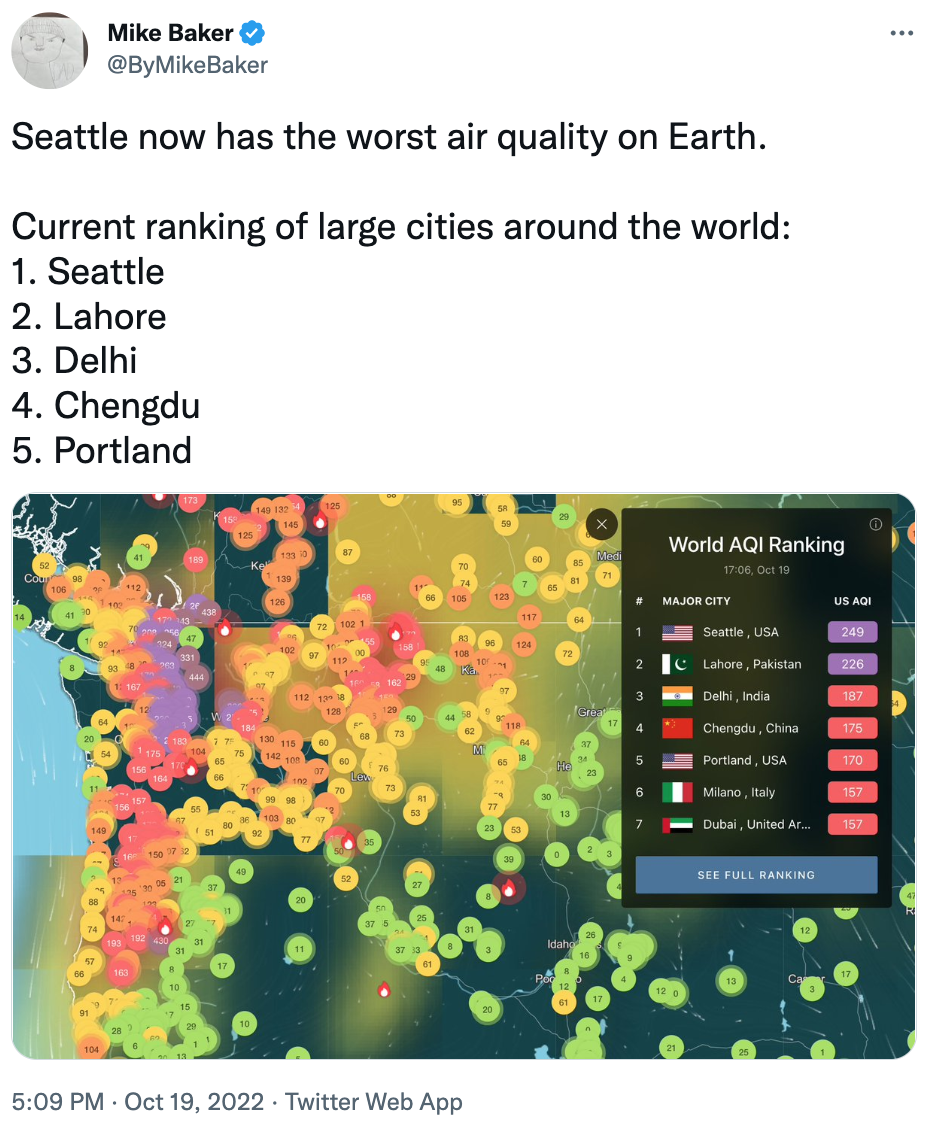
Conditions did not improve the next day. The Space Needle has a webcam (more precisely a “panocam”, as it provides a 360-degree view). Go take a look at it now; this is the grey pall that we embrace for much of the year. Despite this pewter drape, one can still see the surrounding buildings, lakes, and trees. Compare this to the view on October 20th:

(“Is the Mountain Out?” refers to glorious Mt. Rainier, the 14,410-foot tall stratovolcano that looms over the region.)
The rain finally arrived on October 21 and displaced the smoke:

Unfortunately, it did not extinguish the wildfires. Our neighbors to the east have yet to escape the smoke.
In addition to headaches, congestion, and watery eyes, people also experience psychological effects due to wildfires. I came across this paper in Nature Human Behavior from July 2022 that reports on one aspect of this: Exposures and behavioural responses to wildfire smoke (no paywall as of this writing). While the paper doesn’t quite answer the question I want to answer, it did report:
… during large wildfire smoke events, individuals in wealthy locations increasingly search for information about air quality and health protection, stay at home more and are unhappier. Residents of lower-income neighbourhoods exhibit similar patterns in searches for air quality information but not for health protection, spend less time at home and have more muted sentiment responses.
(For those who consider how your digital data gets used, the data for this paper came from Twitter, Google searches, and a real-time air quality monitor called PurpleAir, along with geographic income data.)
As we also have seen during the pandemic, people with lower incomes have less choices, even if they have access to similar information (emphasis mine):
Why do wealthier locations respond differently to smoke exposure? The measured differences do not appear to reflect differences in exposure information or in overall internet activity, given the consistent response of air-quality-related searches across income groups. Rather, the responses are consistent with lower incomes constraining choice sets and behaviours, including less flexibility in working from home, fewer resources with which to consider purchasing protective technology and (regarding the sentiment results) having other more pressing matters to worry about.
The Seattle Times published an article on October 20th that highlighted “constraining choice sets”. The King County Regional Homelessness Authority opened a “smoke shelter“, though few people used it. Why?
“The long-term effects of breathing in smoke is not going to be like the most highest of priority,” said an outreach worker. This is consistent with the findings from the article: While people living outside may have access to the internet, they likely are not seeking air quality monitors or information about filtration, as they do not have their own windows to close or own spaces to filter.
One of the conclusions of the article about wildfires could very well be applied to the pandemic: a “policy approach of promoting private provision of protection could be biased against disadvantaged groups”. I also suspect that the unhappiness the wealthier respondents reported as a result of wildfire smoke is not dissimilar from the ongoing unhappiness we all are seeing as a result of the pandemic and its social consequences. (It is likely that people who are poor are also experiencing unhappiness; they simply may not have the time, energy, or resources to feel it.)


